Search
- Page Path
- HOME > Search
Original Article
- Thyroid
- A Multicenter, Randomized, Controlled Trial for Assessing the Usefulness of Suppressing Thyroid Stimulating Hormone Target Levels after Thyroid Lobectomy in Low to Intermediate Risk Thyroid Cancer Patients (MASTER): A Study Protocol
- Eun Kyung Lee, Yea Eun Kang, Young Joo Park, Bon Seok Koo, Ki-Wook Chung, Eu Jeong Ku, Ho-Ryun Won, Won Sang Yoo, Eonju Jeon, Se Hyun Paek, Yong Sang Lee, Dong Mee Lim, Yong Joon Suh, Ha Kyoung Park, Hyo-Jeong Kim, Bo Hyun Kim, Mijin Kim, Sun Wook Kim, Ka Hee Yi, Sue K. Park, Eun-Jae Jung, June Young Choi, Ja Seong Bae, Joon Hwa Hong, Kee-Hyun Nam, Young Ki Lee, Hyeong Won Yu, Sujeong Go, Young Mi Kang, MASTER study group
- Endocrinol Metab. 2021;36(3):574-581. Published online May 26, 2021
- DOI: https://doi.org/10.3803/EnM.2020.943
- 6,335 View
- 268 Download
- 8 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Postoperative thyroid stimulating hormone (TSH) suppression therapy is recommended for patients with intermediate- and high-risk differentiated thyroid cancer to prevent the recurrence of thyroid cancer. With the recent increase in small thyroid cancer cases, the extent of resection during surgery has generally decreased. Therefore, questions have been raised about the efficacy and long-term side effects of TSH suppression therapy in patients who have undergone a lobectomy.
Methods
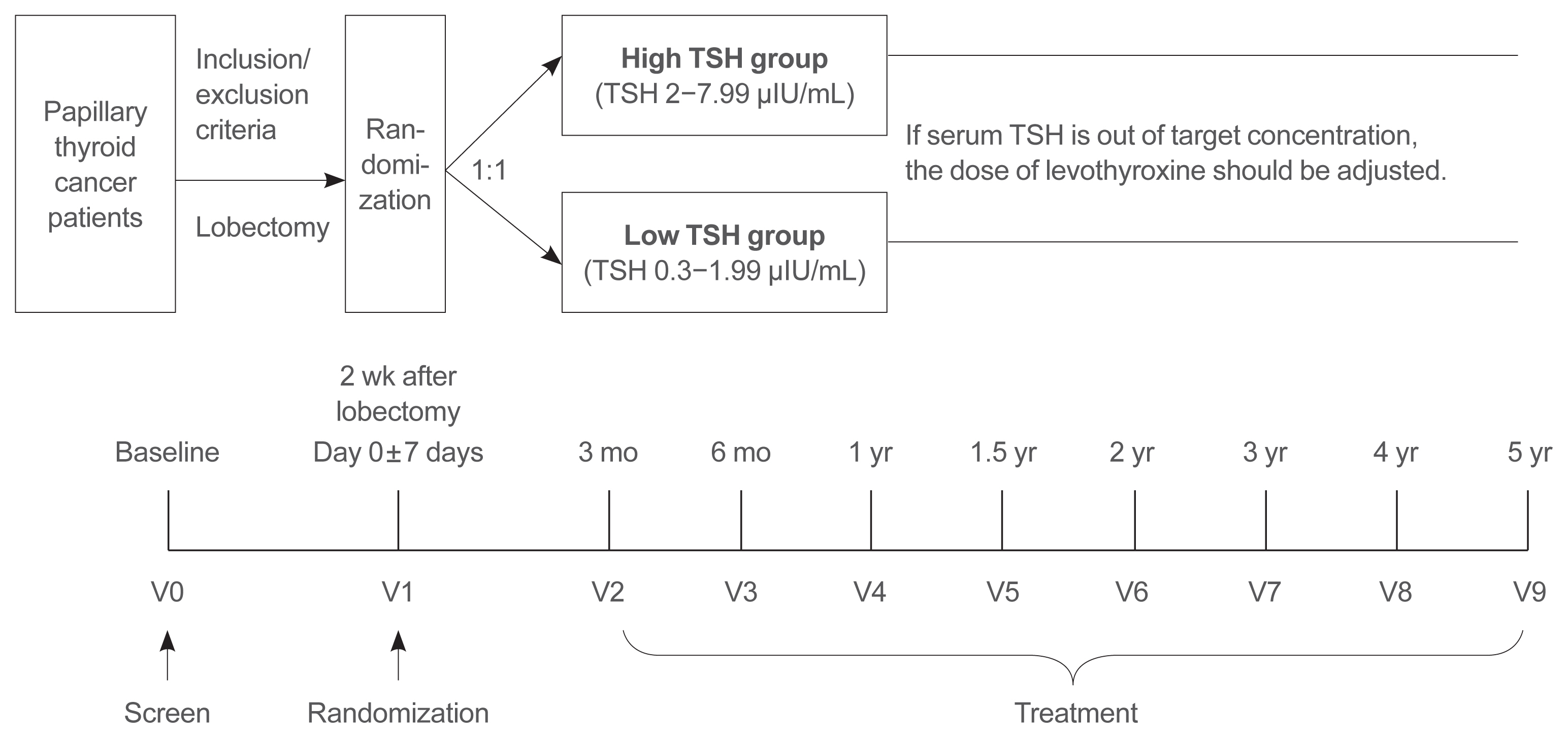
This is a multicenter, prospective, randomized, controlled clinical trial in which 2,986 patients with papillary thyroid cancer are randomized into a high-TSH group (intervention) and a low-TSH group (control) after having undergone a lobectomy. The principle of treatment includes a TSH-lowering regimen aimed at TSH levels between 0.3 and 1.99 μIU/mL in the low-TSH group. The high-TSH group targets TSH levels between 2.0 and 7.99 μIU/mL. The dose of levothyroxine will be adjusted at each visit to maintain the target TSH level. The primary outcome is recurrence-free survival, as assessed by neck ultrasound every 6 to 12 months. Secondary endpoints include disease-free survival, overall survival, success rate in reaching the TSH target range, the proportion of patients with major cardiovascular diseases or bone metabolic disease, the quality of life, and medical costs. The follow-up period is 5 years.
Conclusion
The results of this trial will contribute to establishing the optimal indication for TSH suppression therapy in low-risk papillary thyroid cancer patients by evaluating the benefit and harm of lowering TSH levels in terms of recurrence, metabolic complications, costs, and quality of life. -
Citations
Citations to this article as recorded by- Effect of thyroid-stimulating hormone suppression on quality of life in thyroid lobectomy patients: interim analysis of a multicenter, randomized controlled trial in low- to intermediate-risk thyroid cancer patients (MASTER study)
Ja Kyung Lee, Eu Jeong Ku, Su-jin Kim, Woochul Kim, Jae Won Cho, Kyong Yeun Jung, Hyeong Won Yu, Yea Eun Kang, Mijin Kim, Hee Kyung Kim, Junsun Ryu, June Young Choi
Annals of Surgical Treatment and Research.2024; 106(1): 19. CrossRef - Clinical impact of coexistent chronic lymphocytic thyroiditis on central lymph node metastasis in low- to intermediate-risk papillary thyroid carcinoma: The MASTER study
Da Beom Heo, Ho-Ryun Won, Kyung Tae, Yea Eun Kang, Eonju Jeon, Yong Bae Ji, Jae Won Chang, June Young Choi, Hyeong Won Yu, Eu Jeong Ku, Eun Kyung Lee, Mijin Kim, Jun-Ho Choe, Bon Seok Koo
Surgery.2024; 175(4): 1049. CrossRef - Dynamic Changes in Treatment Response af-ter 131I in Differentiated Thyroid Cancer and Their Relationship with Recurrence Risk Stratification and TNM Staging
璐 狄
Advances in Clinical Medicine.2024; 14(03): 1083. CrossRef - ASO Author Reflections: Active Surveillance may be Possible in Patients with T1b Papillary Thyroid Carcinoma Over 55 Years of Age Without High-Risk Features on Preoperative Examinations
Ho-Ryun Won, Eonju Jeon, Da Beom Heo, Jae Won Chang, Minho Shong, Je Ryong Kim, Hyemi Ko, Yea Eun Kang, Hyon-Seung Yi, Ju Hee Lee, Kyong Hye Joung, Ji Min Kim, Younju Lee, Sung-Woo Kim, Young Ju Jeong, Yong Bae Ji, Kyung Tae, Bon Seok Koo
Annals of Surgical Oncology.2023; 30(4): 2254. CrossRef - Outcomes and Trends of Treatments in High‐Risk Differentiated Thyroid Cancer
Arash Abiri, Khodayar Goshtasbi, Sina J. Torabi, Edward C. Kuan, William B. Armstrong, Tjoson Tjoa, Yarah M. Haidar
Otolaryngology–Head and Neck Surgery.2023; 168(4): 745. CrossRef - Current Controversies in Low-Risk Differentiated Thyroid Cancer: Reducing Overtreatment in an Era of Overdiagnosis
Timothy M Ullmann, Maria Papaleontiou, Julie Ann Sosa
The Journal of Clinical Endocrinology & Metabolism.2023; 108(2): 271. CrossRef - Age-Dependent Clinicopathological Characteristics of Patients with T1b Papillary Thyroid Carcinoma: Implications for the Possibility of Active Surveillance
Ho-Ryun Won, Eonju Jeon, Da Beom Heo, Jae Won Chang, Minho Shong, Je Ryong Kim, Hyemi Ko, Yea Eun Kang, Hyon-Seung Yi, Ju Hee Lee, Kyong Hye Joung, Ji Min Kim, Younju Lee, Sung-Woo Kim, Young Ju Jeong, Yong Bae Ji, Kyung Tae, Bon Seok Koo
Annals of Surgical Oncology.2023; 30(4): 2246. CrossRef - Potential impact of obesity on the aggressiveness of low- to intermediate-risk papillary thyroid carcinoma: results from a MASTER cohort study
Mijin Kim, Yae Eun Kang, Young Joo Park, Bon Seok Koo, Eu Jeong Ku, June Young Choi, Eun Kyung Lee, Bo Hyun Kim
Endocrine.2023; 82(1): 134. CrossRef - Differentiated thyroid cancer: a focus on post-operative thyroid hormone replacement and thyrotropin suppression therapy
Benjamin J. Gigliotti, Sina Jasim
Endocrine.2023; 83(2): 251. CrossRef - Thyroid stimulating hormone suppression and recurrence after thyroid lobectomy for papillary thyroid carcinoma
Mi Rye Bae, Sung Hoon Nam, Jong-Lyel Roh, Seung-Ho Choi, Soon Yuhl Nam, Sang Yoon Kim
Endocrine.2022; 75(2): 487. CrossRef - The Concept of Economic Evaluation and Its Application in Thyroid Cancer Research
Kyungsik Kim, Mijin Kim, Woojin Lim, Bo Hyun Kim, Sue K. Park
Endocrinology and Metabolism.2021; 36(4): 725. CrossRef
- Effect of thyroid-stimulating hormone suppression on quality of life in thyroid lobectomy patients: interim analysis of a multicenter, randomized controlled trial in low- to intermediate-risk thyroid cancer patients (MASTER study)

Case Report
- A Case of Adrenal Teratoma.
- Ji young Kim, Youn zoo Cho, Kang Woo Lee, Dong Mee Lim, Keun Young Park, Byung Joon Kim
- Endocrinol Metab. 2011;26(3):272-275. Published online September 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.3.272
- 65,962 View
- 21 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Teratoma is a congenital tumor containing tissues derived from all germ layers. Teratoma in the region of the adrenal gland is a very uncommon retroperitoneal tumor. Only 7 cases of adrenal teratoma have been reported worldwide, but in Korea, no similar cases have been reported until now. This case report describes an adrenal teratoma in a 38-year-old healthy woman who was incidentally diagnosed with a left adrenal mass on abdominal ultrasonography during a medical inspection. Computed tomographic scans revealed a 9-cm heterogeneous circumscribed round mass, containing primarily fat tissue, and a solid calcification component in the left adrenal gland. Adrenal hormonal assessment results and biochemical markers for gonadal neoplasia were negative. Result of serum laboratory tests were normal. The patient underwent laparoscopic adrenalectomy. Histologic analysis confirmed the diagnosis of a mature teratoma; the obtained specimen measured 5 x 7 x 7.5 cm and weighed 267 g. The surface of the mass was smooth, and sebaceous tissue and hair with hard material were observed on the incisional surface. The patient was discharged on postoperative day 4, without complications. In this case report, we describe the incidental finding of a teratoma occurring in the adrenal gland region in a healthy woman; the teratoma was laparoscopically excised.
-
Citations
Citations to this article as recorded by- Lipomatous tumours in adrenal gland: WHO updates and clinical implications
Alfred King-yin Lam
Endocrine-Related Cancer.2017; 24(3): R65. CrossRef - A Case of Teratoma of Thyroid Gland in Adolescence
Yu-Chang Lee, Su-Jin Jeong, Sol-Jae Lee, Chong-Hwa Kim, Yong-Hoon Lee, Jung-Eun Lee, Hye-Ji Seo
International Journal of Thyroidology.2017; 10(1): 61. CrossRef
- Lipomatous tumours in adrenal gland: WHO updates and clinical implications

Original Article
- GLP-1 Can Protect Proinflammatory Cytokines Induced Beta Cell Apoptosis through the Ubiquitination.
- Dong Mee Lim, Ju Young Kim, Kang Woo Lee, Keun Young Park, Byung Joon Kim
- Endocrinol Metab. 2011;26(2):142-149. Published online June 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.2.142
- 1,625 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Proinflammatory cytokines are one of the causes of diabetes mellitus. However, the exact molecular mechanism by which proinflammatory cytokines induce beta-cell death remains to be clearly elucidated. Glucagon-like peptide-1 (GLP-1) affects the stimulation of insulin secretion and the preservation of beta-cells. Additionally, it may exert an antiapoptotic effect on beta cells; however, the mechanism underlying this effect has yet to be demonstrated. Therefore, we investigated the protective effects of GLP-1 in endoplasmic reticulum (ER)-mediated beta-cell apoptosis using proinflammatory cytokines. METHODS: To induce ER stress, hamster insulin-secreting tumor (HIT)-T15 cells were treated using a mixture of cytokines. Apoptosis was evaluated via MTT assay, Hoechst 33342 staining, and annexin/propidium iodide (PI) flow cytometry. The mRNA and protein expression levels of ER stress-related molecules were determined via PCR and Western blotting, respectively. Nitric oxide was measured with Griess reagent. The levels of inducible nitric oxide synthase (iNOS) mRNA and protein were analyzed via real-time PCR and Western blot, respectively. iNOS protein degradation was evaluated via immunoprecipitation. We pretreated HIT-T15 cells with exendin (Ex)-4 for 1 hour prior to the induction of stress. RESULTS: We determined that Ex-4 exerted a protective effect through nitric oxide and the modulation of ER stress-related molecules (glucose-regulated protein [GRP]78, GRP94, and CCAAT/enhancer-binding protein homologous protein [CHOP]) and that Ex-4 stimulates iNOS protein degradation via the ubiquitination pathway. Additionally, Ex-4 also induced the recovery of insulin2 mRNA expression in beta cells. CONCLUSION: The results of this study indicate that GLP-1 may protect beta cells against apoptosis through the ubiquitination pathway.

Case Reports
- A Case of Coexistence of Parathyroid and Papillary Thyroid Carcinoma.
- Yoon Shick Yom, Myung Jun Lee, Hyun Woo Lim, Jeong Ho Park, Sung Tae Kim, Yu Mi Lee, Dong Ju Yang, Youn Zoo Cho, Moon Il Park, Kang Woo Lee, Keun Young Park, Dong Mee Lim, Byung Joon Kim
- J Korean Endocr Soc. 2010;25(1):61-67. Published online March 1, 2010
- DOI: https://doi.org/10.3803/jkes.2010.25.1.61
- 1,660 View
- 25 Download
-
 Abstract
Abstract
 PDF
PDF - Primary hyperparathyroidism is usually caused by a parathyroid adenoma, occasionally by primary parathyroid hyperplasia and rarely by parathyroid carcinoma. Coincidental occurrence of thyroid carcinoma in parathyroid adenoma is not uncommon, but synchronous parathyroid and thyroid carcinoma is extremely rare. Here, we describe a case of synchronous parathyroid carcinoma and papillary thyroid carcinoma.

- A Case of Prolonged Hypoglycemia Post Topiramate Treatment an Anti-convulsant, in a Type 2 Diabetic Patient.
- Myung Jun Lee, Yoon Shick Yom, Hyun woo Lim, Sung Tae Kim, Yu Mi Lee, Youn Zoo Cho, Kang Woo Lee, Byung Joon Kim, Keun Young Park, Dong Mee Lim
- J Korean Endocr Soc. 2009;24(4):277-280. Published online December 1, 2009
- DOI: https://doi.org/10.3803/jkes.2009.24.4.277
- 3,738 View
- 93 Download
-
 Abstract
Abstract
 PDF
PDF - Topiramate is a drug used to treat epilepsy, and is known for its effects including reduced appetite resulting in lower body weight, and the lowering of neutral fat. In addition, topiramate is known to reduce blood sugar levels by increasing insulin sensitivity and by increasing insulin secretion by glucose stimulation. The authors report a case of persistent hypoglycemia, in a patient who had been administrating topiramate, as a treatment for epilepsy following an episode of cerebral infarction.

- A Case of Adrenocortical Carcinoma with Concurrent Cushing's Syndrome and Primary Aldosteronism.
- Chang Won Lee, Hyun Ju Yoon, Won Min Hwang, Jung Kyu Kim, Hoon Sup Koo, Dong Mee Lim, Eu Gene Choi, Moon Jun Na, Do Yeun Cho, Bum Kyeong Kim, In Seok Choi, Keun Young Park
- J Korean Endocr Soc. 2004;19(4):446-451. Published online August 1, 2004
- 1,149 View
- 20 Download
-
 Abstract
Abstract
 PDF
PDF - An adrenocortical carcinoma is a rare malignancy, which is associated with a poor prognosis. Eighty percent of adrenal tumors are functional, and commonly secrete glucocorticoids alone (45%), glucocorticoids and androgens (45%) or androgen alone (10%). Less than 1% of all cases secrete aldosterone. A case of a 75 year old female patient was experienced, presenting with anadrenocortical carcinoma and associated concurrent Cushing's syndrome and primary aldosteronism. She had complained of left flank pain for 5 months, and also showed clinical features of Cushing's syndrome, hypertension, hypokalemia and a left abdominal mass. An abdominal CT* demonstrated a large left adrenal mass, with necrosis, and a hemorrhage in the left upper abdomen. The plasma renin activity was 0.51 ng/ml/hr, and the serum aldosterone level was increased by 46.4 ng/dL. A low and high dose dexamethasone suppression test revealed no suppression. Histologically, the tumor was diagnosed as a adrenocortical carcinoma. After complete removal of the mass, she received mitotan and prednisolone as adjuvant therapies. Liver and bone metastasis occurred after 6 months of treatment, so was treated with palliative radiotherapy for the bone metastasis


 KES
KES

 First
First Prev
Prev



